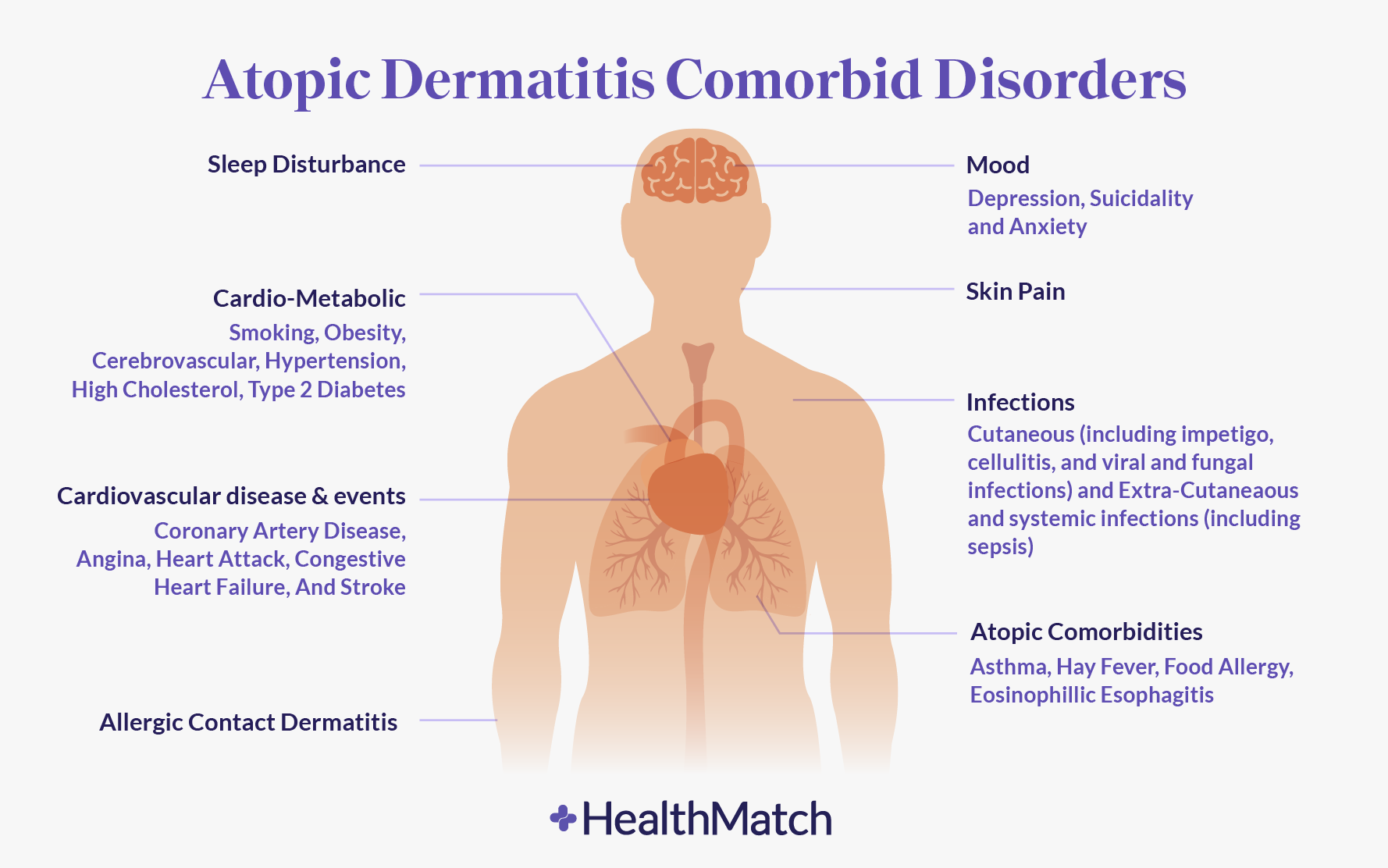
The Mental Health Burden of Atopic Dermatitis: Atopic dermatitis, the most common form of eczema, is often thought of as “just a skin condition,” but for millions of people, its impact reaches far deeper. Affecting up to 25% of children and 10% of adults worldwide, this chronic inflammatory disorder brings more than rashes and relentless itch—it introduces daily struggles with self-confidence, social interactions, and overall emotional well-being. Patients often describe sleepless nights, constant discomfort, and embarrassment from flare-ups that can appear anywhere on the body. These physical symptoms alone can leave a profound psychological mark.
Understanding the Link Between Atopic Dermatitis and Mental Health
Psychological Strain of a Visible Disease
A visible condition like atopic dermatitis can erode self-esteem. Flare-ups on the face, hands, or arms make many patients feel self-conscious in public, avoiding social gatherings or relationships. This avoidance can lead to loneliness, anxiety, and depression, creating a cycle where mental health symptoms worsen physical ones.
Read about: The Mental Health Burden of Atopic Dermatitis
Role of Sleep in Worsening Neuropsychiatric Outcomes
Sleep Disruption as a Mediator
One of the strongest connections between atopic dermatitis and mental health is poor sleep quality. Studies show that individuals with atopic dermatitis are two to four times more likely to experience sleep disorders such as insomnia or sleep apnea. The itch-scratch cycle often prevents children and adults alike from falling or staying asleep.

Also read: Suzuki e-Access Price Reveal Soon – 95km Range, Rival to iQube & Rizta
Untangling Cause and Effect
Despite growing evidence, it remains difficult to determine whether atopic dermatitis causes mental health issues or simply shares overlapping risk factors with them. Social isolation, poor sleep, and inflammatory processes all contribute, but the precise mechanisms are still unclear. Large-scale, long-term studies such as the PEDISTAD international study, which follows children with moderate-to-severe atopic dermatitis over ten years, aim to shed light on whether early treatment can prevent later psychiatric diagnoses.
FAQs
1. Why does atopic dermatitis affect mental health?
Atopic dermatitis affects mental health through both psychological and biological pathways. The visible nature of the disease can reduce confidence, while constant itching disrupts sleep and daily life. Biologically, inflammation and immune dysregulation may also influence brain function, contributing to anxiety, depression, or ADHD-like symptoms.
2. What mental health conditions are most common in people with atopic dermatitis?
The most common conditions include anxiety and depression, but studies also show higher risks of ADHD, OCD, cognitive and behavioral changes, and alexithymia. Children with severe eczema are especially vulnerable to developmental and attention-related diagnoses.